Research on Pulmonary Toxicity
Hyperbaric oxygen treatment and pulmonary function
By F. POTT, P. WESTERGAARD, J. MORTENSEN, and E. C. JANSEN
The Hyperbaric Treatment Unit. Center of Head and Orthopedics, Clinic of Operations and Anesthesia,; and Department of clinical Physiology. Rigshospitalet, University of Copenhagen, Blegdamsvej 9, DK-2100 Copenhagen 0, Denmark
Pott F, Westergaard P, Mortensen J, Jansen EC. Hyperbaric oxygen treatment and pulmonary function. Undersea Hyper Med 1999; 26(4 ):225-228.-Hyperbaric oxygen (HBO2) treatment exposes the lungs to the potentially toxic effect of free oxygen radicals and may lead to impairment of pulmonary function. HBO2 significantly improves wound healing in patients with osteoradionecrosis of the mandible following radiation therapy for intraoral cancer. In 18 consecutive patients with osteoradionecrosis of the mandible, pulmonary function was assessed during 6 wk of HBO2 treatment, applied daily in a monoplace chamber for 90 rnin and at a partial oxygen pressure of 2.4 atm abs. Pretreatment forced vital capacity (FVC) was 104 + 14% (mean + SD) of a reference population, the 1 s forced expiratory volume (FEV1) 95 + 20%, total lung capacity (TLC) 100 + 13%, and the carbon monoxide diffusing capacity (DLco) 81 + 17% (P< 0.05, compared to reference population). These parameters remained unchanged throughout the treatment period (after 6 wk and expressed relative to the percentage of the expected value at baseline): delta FVC: +4 + 8%; delta FEV1: -2 + 4 %; delta TLC: +2 + 5%; delta DLco: 0 + 9%; delta RV 0 + 11%. It is concluded that intermittent HBO2 treatment in a monoplace chamber has no persistent effect on pulmonary function and can be offered even to patients with a reduced diffusing capacity.
hyperbaric oxygenation, lung function, osteoradionecrosis, smoking
Oxygen has a toxic potential due to the production of free radicals (1,2). Oxygen-induced tissue damage is reported for most organs (3-4) and this has to be considered when patients are exposed to an elevated oxygen concentration and pressure. Exposure to oxygen is highest for lung tissue because partial oxygen pressure (PO2) is higher in the alveoli than in the arteries. Consequently, several studies reported a reduced pulmonary function following hyperbaric oxygen (HBO2) therapy, and the incidence increases both with the inspiratory partial pressure and the time of exposure (4-6).
Hyperbaric oxygen treatment at a partial oxygen pressure of 2.4 atm abs for 6 wk and with a duration of 5 times 90 min/wk improves wound healing in patients with osteoradionecrosis of the mandible after radiation therapy for intraoral cancer (7). Marx and Johnson (8) demonstrated HBO2 induced fibroplasia and angiogenesis in the radiated tissue.
The objective of this study was to investigate the effect of this HBO2 protocol on pulmonary function as assessed by standard pulmonary function testing.
METHODS
Five females and 13 males, with a mean age of 57 yr (range 48-79), weight 61 kg (46-99), and height 164 cm (159-190), underwent surgery for intraoral squamous cell carcinoma and developed osteoradionecrosis of the mandible after radiation therapy. The patients were three non-smokers, six moderate smokers (<20 cigarettes/day), and nine heavy smokers (>20 cigarettes/day).
Hyperbaric oxygen treatment encompassed 30 sessions (5/wk) ina monoplace pressure chamber (Vickers Oxy-genaire LDT, Hampshire, England) with a compression/decompression time of 5 and 90 min continuous exposure to 2.4 atm abs at 100% inspiratory oxygen. As part of the routine monitoring in our HBO2 treated patients, forced vital capacity (FVC), 1 s forced expiratory volume (FEV1), total lung capacity (TLC), single-breath carbon-monoxide diffusing capacity (DLco), peak flow, and residual volume (RV) were assessed initially and weekly throughout the treatment period at least 20 h after the preceding session (Jaeger Masterlab, Jaeger, Germany). The equipment fulfills the accuracy criteria established by the European Respiratory Society (9) and American Thoracic Society (10).The maneuvers were performed as recommended in the guidelines (9,10). At least three technically acceptable forced expirations were obtained. The largest FEV1 and the largest FVC (not exceeding the second largest by more than 5% or 100 ml) were used. The average of two technically acceptable single-breath measurements of DLco ThC, and RV were used (reproducibility requirements are met if each result differs less than 10% from the average). At routine follow-up, only one measurement of DLco and TLC was performed if the result was within 10% of the previous result; however, if it differed more than 10% at least two measurements were obtained.
Data are expressed as mean with standard deviation and related to data from a reference population adjusted for age, sex, and height (9). Friedman's analysis of variance was employed to determine differences with time. A P<0.05 was considered significant.
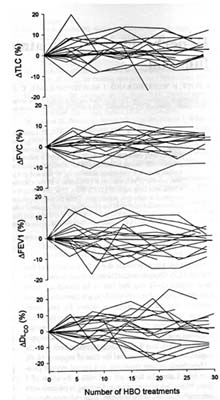
FIG. 1 - Individual course of TLC, TVC, FEV1, and DLco before and during ~ 6 wk of HBO2 treatment.
RESULTS
Pretreatment FVC was 4.1 + 1.2 liter or 104 + 14% (mean + SD) of the reference values, FEV1 3.0 + 1.0 liter (95 + 20%), TLC 6.5+ 1.4l (100 + 13%), and DLco 7.5 + 2.2 liter . min-1. kpa-1 (81 + 17%; P <0.05),RV 2.3 + 0.5 l (103 + 23%), peak flow 6.4 + 1.9 liter min-1 (82 + 19%; P <0.05),and FEV1/FVC 73 + 8% (97 + 11%). These parameters remained unchanged throughout the treatment period. After 6 wk and expressed relative to the percentage of the expected value at baseline: delta FVC: + 4 + 8%; delta FEV1: -2 + 4%; delta TLC: +2 + 5%; delta DLco: 0 + 9%; delta RV 0 + 11%, delta peak flow + 2 + 19%; delta FEV1/FVC –5 + 7% (Fig, 1, Table 1). After 6 wk of treatment the largest individual reduction detected in FVC and TLC were - 9 % and - 8 %, respectively. No difference in the time course of any variable was detected when patients were divided into two groups according to a pretreatment DLco above or below 70% of the reference value.
DISCUSSION
This study evaluated the effect of intermittent HB02 therapy on pulmonary function as assessed by standard pulmonary function testing. No persistent effect could be detected in patients with previously impaired diffusing capacity, indicating that a HBO2 treatment protocol with 90 min continuous exposure to 2.4 atm abs oxygen partial pressure on a daily basis is safe for the lungs. We did not investigate the short-term effect of HB02 treatment because measurements were taken about 20 h after the last session and it cannot be excluded that the applied protocol leads to immediate but temporary pulmonary impairment.
With a similar P02 (2.5atm abs) and an exposure duration of 6 h, Clark (5) found a 14% postexposure reduction of the FVC, a 31% reduction of the maximal middle expiratory flow, and an 8% change in the diffusing capacity. Such changes may persist for several days because after ~11 h exposure to 2.0 atm abs, vital capacity gradually recovered over 11 days (6). After daily HBO2 sessions (90 min at 2.4 atm abs), and 4 wk after the end of treatment, Thorsen et al. (11) found patients with normal pretreatment pulmonary function small but significant reduction in mean forced mid – expiratory flow rate (~10%) indicating a small reduction in small airway conductance. Before the last treatment the authors found DLco reduced by 4%. We agree that such reduction in pulmonary function is not considered to be of clinical significance.
Table 1: Pulmonary Function During Hyperbaric Oxygen Treatment
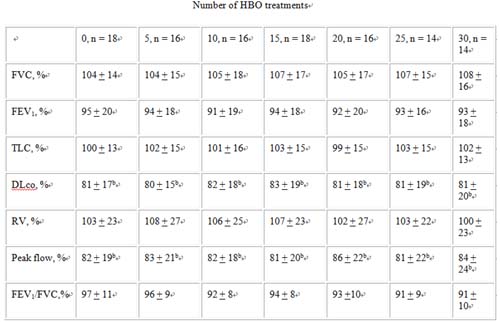
FVC, FEV1, mc, DLco, RV, peak flow, and ratio of FEV1 and FVC (FEV1/FVC) during -6 wk of HBO2 treatment. Values are mean + SD and related to a reference population adjusted for age, sex, and height.
b) significant difference from reference population, P <0.05.
The diffusing capacity is affected by duration of exposure rather than the partial pressure (12-14). Clark and Lambertsen (12) defined a Unit of Pulmonary Toxic Dose (UPTD) as
UPTD = t(2(PO2 - .5))5/6
where t = exposure time. They found a 2% decrease of VC at a UPTD of 615, and a l0% decrease at a UpTD of 1,425. Accordingly, in our study, a single treatment was at a UPTD of 273, and it was 8,208 units for the total series of 30 treatments. The present results support the finding that the dose effect of intermittent exposure is largely reduced and therefore the cumulative UPTD is different from the UPTD from continuous exposure (15).It could be speculated that the treatment protocol induces temporary changes in pulmonary function, as measurements were undertaken about 20 h post exposure. However, no significant differences were found when pulmonary function was assessed daily for 5 days before and after two intervals of 40 min HB02 exposure at 2.5atm abs, separated by a 5-min air break (16).
We investigated our patients in a monoplace chamber where oxygen was breathed freely and continuously. We do not know whether the work of breathing is greater through a mask, but we expect that multiplace chamber treatment at the same pressure and minutes of oxygen but including air breaks would give the same results.
In most of our patients, diffusing capacity was impaired before treatment was started and this may be because most of them are or have been heavy smokers. Smoking is known to reduce oxygen radical tolerance (17), and we take the unchanged pulmonary function in these patients to suggest that the applied HBO2 treatment protocol is safe even in lungs with a reduced diffusing capacity.
We thank Jens Thorn, associate professor, Department of Oral and Maxillofacial Surgery and the staff of the Department of Clinical Physiology, Rigshospitalet, Copenhagen, Denmark, for their contribution to this work. We are grateful for the critical review of Professor Asger Dierksen, Depmtment of Infectious Diseases, Rigshospitalet.
REFERENCES
1. Gerslunan R. Biological effects of oxygen. In: Dickens F, Neil E, eds. Oxygen in the animal organism. New York: Macmillian, 1964:475-494.
2. McCord JM, Fridovich I. The biology and pathology of oxygen radicals. Ann Intern Med 1978; 89:122-127.
3. Lambertsen CJ. Effects of hyperoxia on organs and their tissues. In: Robin ED, ed. Extrapulmonary manifestations of respiratory disease. Volume 8 of Lung biology in health and disease. Edited by C. Lenfant. New York: Marcel Dekker, 1978:239-303.
4. Clark JM. Oxygen toxicity. In: Bennet RB, Elliot DH, eds. The physiology and medicine of diving. London: WB Saunders 1993: 122-169.
5. Clark JM. Pulmonary limits of oxygen tolerance in man. Exp Lung Res 1988; 14:897-910.
6. Clark JM, Lambertsen CJ. Rate of development of pulmonary oxygen toxicity in man during oxygen breathing at 2.0 ATA. J Appl Physiol 1971; 30:739-752.
7. Thornn JJ, Kallehave F, Westergaard P, Hjorting HE, Gottrup F. The effect of hyperbaric oxygen on irradiated oral tissues: transmucosal oxygen tension measurements. J Oral Maxillofac Surg 1997;55:1103-1107.
8. Marx RE, Johnson RP. Studies in the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg 1987; 64:379-390.
9. Standardized lung function testing: Official Statement of The European Respiratory Society. Eur Respir 3 1993; 6(suppl 16):1-100.
10. Official statement of ATS. Single-breath carbon monoxide diffusing capacity (transfer factor). Recommendations for a standard technique -1995 update. Am J Respir Crit Care Med 1995;152:2185-2198.
11. Thorsen F, Aanderud L, Aasen Tb. Effects of a standard hyperbaric oxygen treatment protocol on pulmonary function. Eur Respir 3 1998; 12(6):1442-1445.
12. Clark JM, Lambertsen CJ. Pulmonary oxygen toxicity: a review. Pharm Rev 1971; 23:27-133.
13. Caldwell PRB, Lee WL Jr., Schildkraut HS, Archibald ER. Changes in lung volume, diffusion capacity, and blood gases in man breathing oxygen. J Appl Physiol 1966; 21:1477-1483.
14. Puy RJM, Hyde RW, Fisher AB, Clark JM, Dickson J, Lambertsen CJ. Alterations in the pulmonary capillary bed during early 02 toxicity in man. J AppI Physiol 1968; 24:537-54
15. Hendricks PL, Hall DA, Hunter WL Jr, Haley PJ. Extension of pulmonary oxygen tolerance in man at 2 ATA by intermittent oxygen exposure. J Appl Physiol 1977; 42:593-599.
16. Shupak A, Abramovich A, Adir Y, et al. Effects on pulmonary function of daily exposure to dry or humidified hyperbaric oxygen. Respir Physiol 1997; 108:241-246.
For those interested in receiving HBOT that may have difficulty with financing the treatments, we have people that can give advice on fund-raising. The previous case studies are only a glimpse of the hundreds of people which have received HBOT at the Richmond Hyperbaric Center for a variety of conditions with favorable outcomes. Please contact us for more information on a particular condition which may benefit from hyperbaric oxygen therapy.
The Richmond Hyperbaric Health Center has engaged in scientific research projects including a pilot study on the treatment of RSD/CRPS. We would like to pursue future research studies as well and are open to any inquiries about the use of HBOT for researching various conditions.

